If you live with autoimmune disease, stubborn digestive issues, or mystery symptoms that never quite resolve, there’s a good chance dysbiosis, leaky gut, and inflammation are quietly driving the bus. These form a classic trifecta: dysbiosis (imbalanced gut microbes), increased intestinal permeability (leaky gut), and chronic inflammation that feed off each other in a vicious cycle
Until you address all three, true healing is hard to come by, but the good news is: with the right tools—healing the gut lining, rebalancing the microbiome, and adopting an anti-inflammatory lifestyle—you can start turning that cycle around.
I don’t come to this topic as a distant clinician; I come as someone who has lived it. I’ve battled leaky gut, dysbiosis, and inflammation for years alongside autoimmune disease, and I’ve seen firsthand how much they affect everything from my digestion to my energy, mood, and brain function. For those with active autoimmune disease, leaky gut is likely present, whether they know it or not.
I healed my leaky gut years ago but took another hit when I experienced uranium toxicity. That layer of toxic burden pushed an already-fragile system back over the edge, and many of my symptoms flared again. This supports the fact that you can’t separate environmental exposure from gut health and inflammation.
As a child, I took several rounds of antibiotics for ear infections. Then, in college, I spent about three years on minocycline for perioral dermatitis. It kept the rash under control but quietly disrupted my microbiome the entire time. I even had to use Monistat weekly to keep yeast in check. Then, almost as soon as I graduated and passed the CPA exam, the dermatitis disappeared. Can you say stress-driven? Yes. It’s all connected.
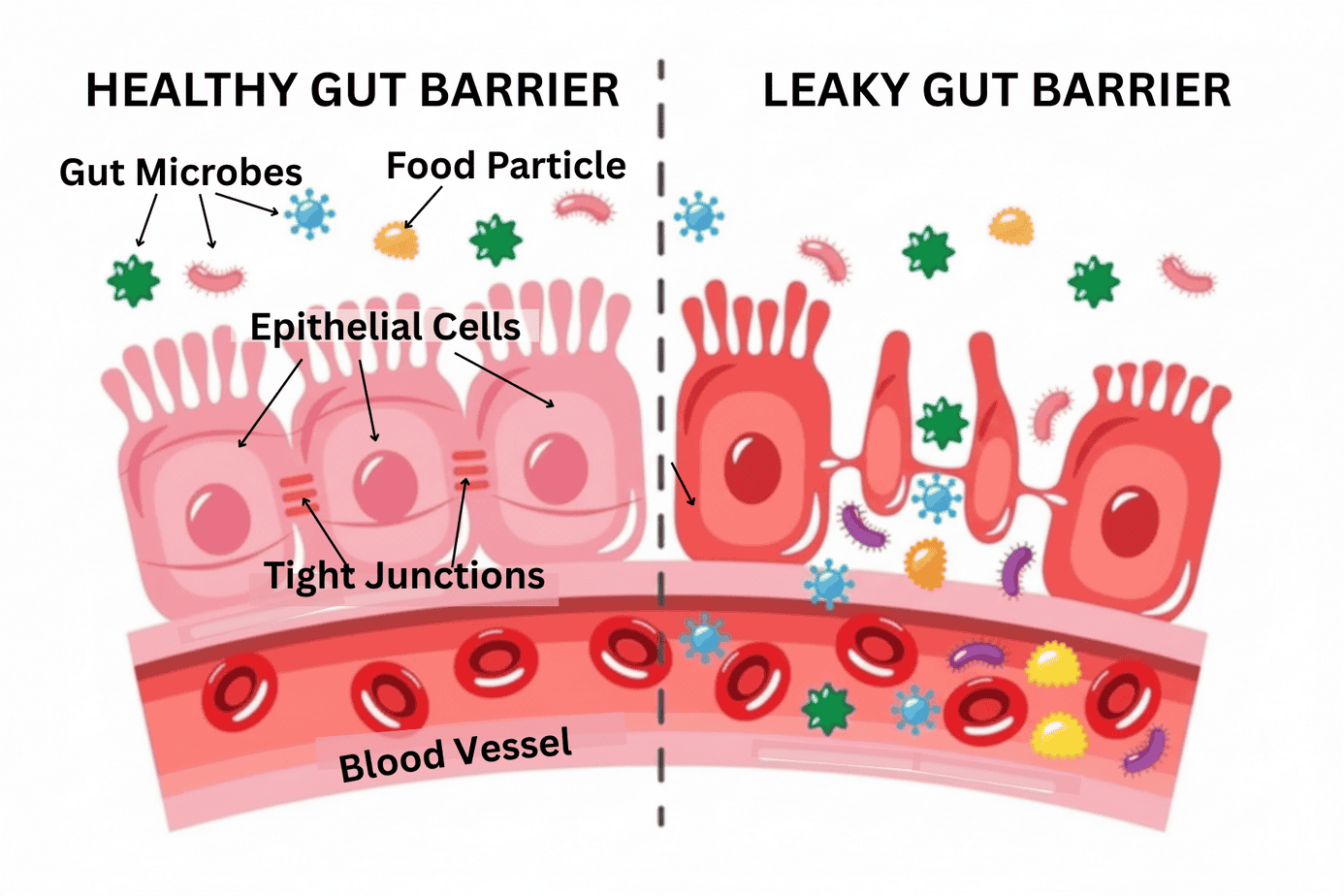
What Is Leaky Gut?
Leaky gut, or increased intestinal permeability, is what happens when the tight junctions between cells in your gut lining loosen. Instead of acting like a well-guarded gate that lets small nutrients out into the bloodstream, your gut becomes more of a leaky sieve that lets large fragments out. Undigested food particles, bacterial fragments, and toxins that should stay inside the digestive tract can slip into the bloodstream, triggering an inflammatory immune response.
You can read more about leaky gut, its symptoms, what causes it, and why it matters in this post: Intestinal Permeability: What Leaky Gut Really Is (and Isn’t)
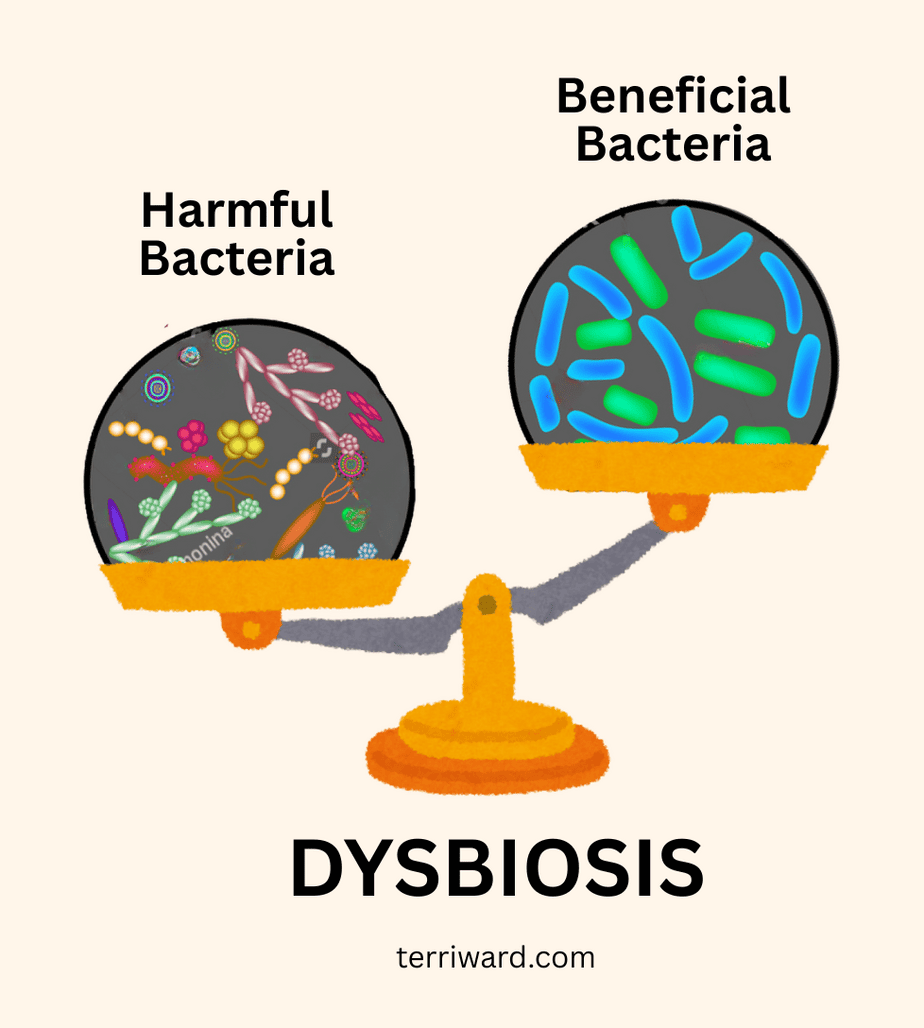
What Is Dysbiosis?
Dysbiosis is an imbalance in the microbes that live in and on us—including bacteria, yeast, viruses, and other organisms in the gut. In a healthy gut, these communities exist in a dynamic but symbiotic relationship. Beneficial bacteria keep opportunistic ones in check, produce compounds your body needs, and help regulate your immune system.
Dysbiosis is what happens when that balance breaks down. It isn’t simply about “good” versus “bad” microbes; it’s about a loss of microbial diversity, a reduction in beneficial species, and an overgrowth of bacteria or fungi that, in excess, cause harm. You can have dysbiosis without obvious digestive symptoms, which is part of what makes it so easy to miss.
Common contributors include:
-
- Antibiotics and other medications (NSAIDs, statins, antidepressants, acid blockers)
- Poor diet (highly processed foods, low fiber, high sugar)
- Chronic stress
- Sleep deprivation
- Environmental toxins, including heavy metals
Antibiotics are sometimes necessary and absolutely can save lives. Yet they’re a blunt instrument. They don’t only target the “problem” bacteria; they affect the entire microbial community. If that ecosystem isn’t rebalanced—and the other contributing factors aren’t addressed—even a single round of antibiotics can tip the scale from resilient health toward dysbiosis and symptoms.
In my own case, years on minocycline, the stress of being a single parent, student, and tax preparer, and an impending CPA exam with the highest failure rate of any professional exam created a perfect storm for dysbiosis.
You can read more about dysbiosis in this article I wrote: Dysbiosis: A Microbial Imbalance with 5 Treatment Strategies
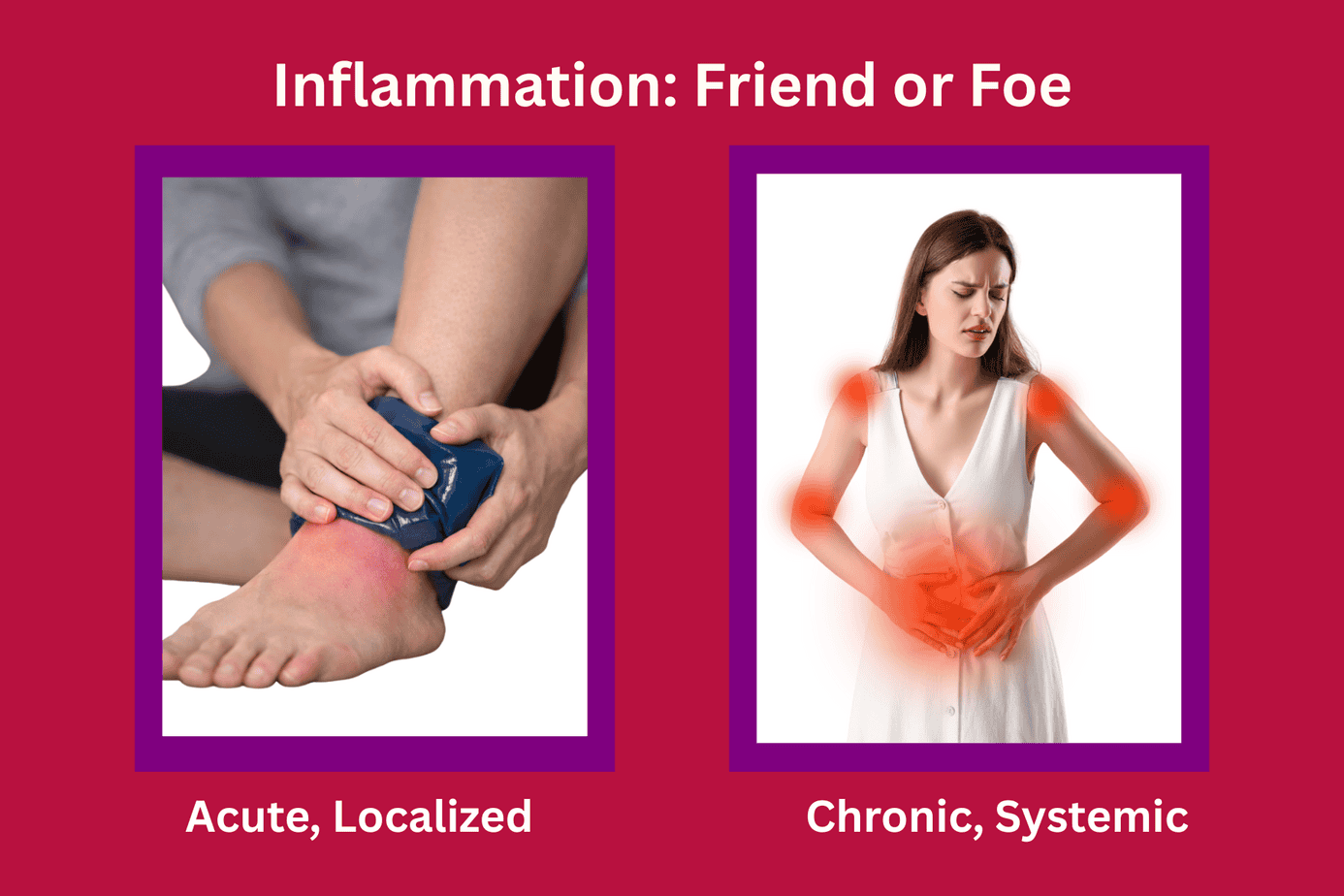
Chronic Inflammation’s Role
Inflammation isn’t our enemy; we need it to fight infections and heal injuries. The problem is chronic, low-grade inflammation that never really turns off. It’s that smoldering inflammation operating quietly in the background, slowly damaging tissues and systems throughout the body that is central to the development and progression of most chronic diseases.
Chronic inflammation driven by gut dysfunction has been linked to:
-
- Nearly every autoimmune condition, including celiac disease, Crohn’s disease, Hashimoto’s, rheumatoid arthritis, and lupus
- Metabolic dysfunction and insulin resistance
- Obesity and difficulty losing weight
- Cardiovascular disease
- Neurological conditions, including neuropathy, depression, and cognitive decline
- Skin disorders such as eczema and psoriasis
- Food sensitivities, which often develop as the immune system becomes hyperreactive to proteins crossing a compromised barrier
When leaky gut and dysbiosis are present, your immune system is continually nudged: “Something’s wrong, stay on guard.” That leads to:
-
- Higher levels of inflammatory messengers
- More immune confusion and self-tissue attack in autoimmune conditions
- Greater wear and tear on tissues and mitochondria (the organelles in our cells that produce energy)
This is not a fringe theory. The connection between dysbiosis, and leaky gut, inflammation is well-documented in peer-reviewed literature. It’s just not yet reflected in most conventional medical appointments because there’s no quick-fix drug to mask symptoms and no billing code to justify the time it takes to address it.
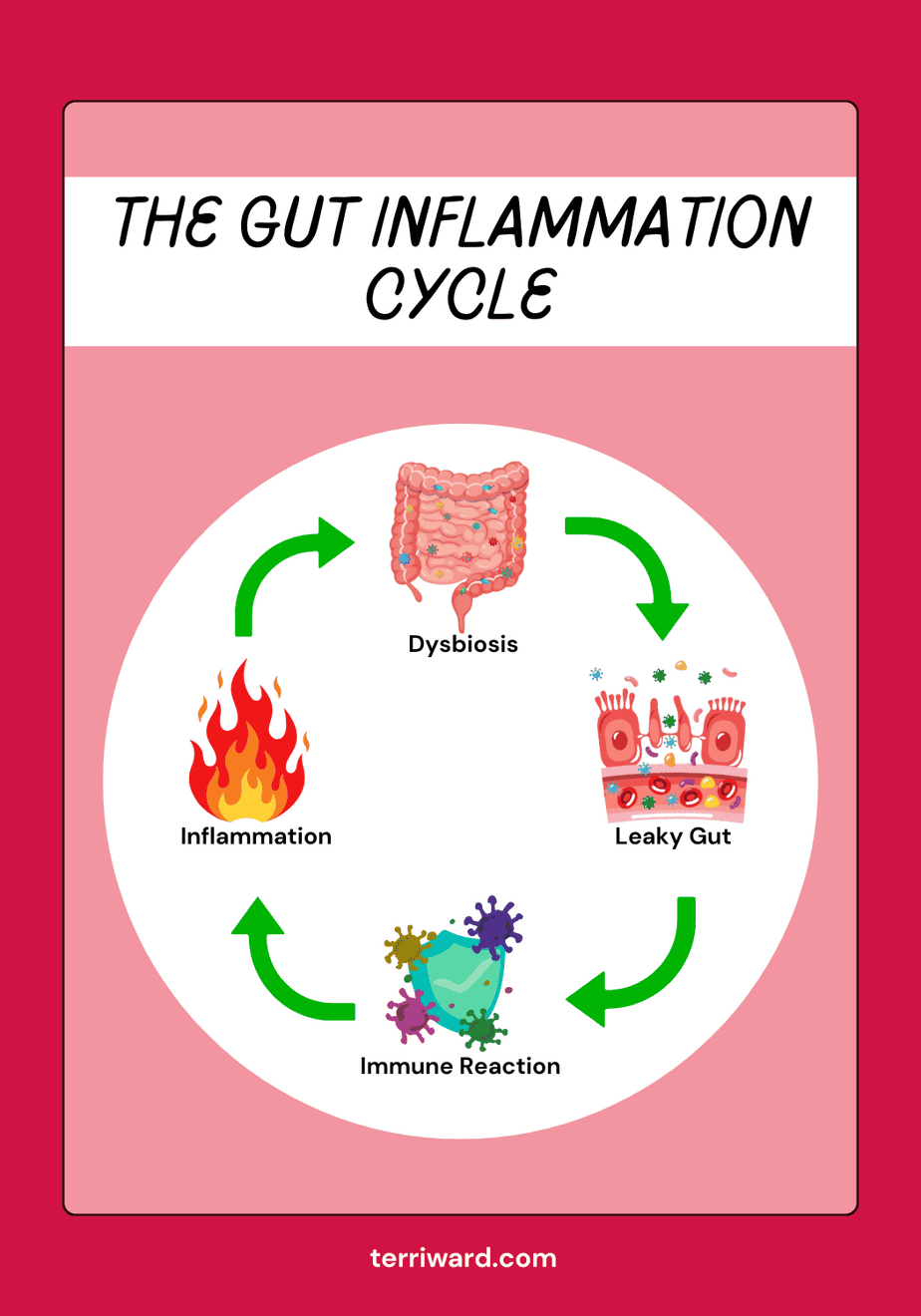
How Dysbiosis, Leaky Gut, and Inflammation Feed Each Other
The components of this triad don’t just coexist—they create and feed each other in a feedback loop. Here’s how the loop perpetuates itself:
1. Dysbiosis irritates and inflames the gut lining.
Harmful or overgrown microbes can produce irritating byproducts, crowd out protective species, and thin the mucus layer that shields the gut lining. When beneficial bacteria are reduced, the gut loses some of its most important defenders. Short-chain fatty acids (SCFAs)—especially butyrate, the primary fuel source for the cells lining the colon—are produced when healthy gut bacteria ferment dietary fiber. When SCFA production drops, the intestinal barrier weakens.
2. An irritated gut lining becomes leaky.
The tight junction proteins that act as gatekeepers between your gut and bloodstream begin to loosen, allowing larger particles to cross the gut barrier. Bacterial fragments, including an endotoxin known as lipopolysaccharide (LPS), can slip into the bloodstream along with undigested food particles.
3. Your immune system sees those particles as invaders.
It treats these particles as a serious threat and mounts an inflammatory response, both locally in the gut and systemically throughout the body. In the short term, that response is appropriate, but when the leakage continues, the immune response does too.
4. Systemic inflammation further damages the gut and microbiome.
Here’s how the loop continues: inflammation further disrupts the microbiome, which worsens leaky gut, which allows more LPS and other particles to leak through, which drives even more inflammation. Inflammatory chemicals, stress hormones, and oxidative stress all make it harder for the gut lining to heal and for beneficial microbes to thrive.
5. The cycle continues—unless we intervene.
Around and around it goes, often for years, while symptoms accumulate until the root causes are addressed.
For anyone with autoimmune disease, chronic pain, metabolic issues, or even sepsis, this loop is almost always running in the background. The goal is not perfection; it’s interrupting the loop at multiple points so the body can start to repair instead of living in a perpetual inflammatory feedback cycle.
What This Means for Autoimmune Conditions and Food Sensitivities
If you have an autoimmune condition, this cycle is especially relevant. A large portion of the immune system—often estimated at 70 to 80%—resides in and around the gut. Therefore, chronic dysbiosis, leaky gut, and inflammation keep that immune tissue in a state of constant activation. For someone with an already overreactive immune response, this is like pouring fuel on a fire.
Research shows evidence of increased intestinal permeability in virtually every autoimmune condition studied, often years before an official diagnosis. That doesn’t mean leaky gut causes autoimmunity in every case. The relationship is complex and bidirectional. However, it does suggest that gut barrier integrity is a critical piece of the puzzle when it comes to managing and possibly quieting autoimmune activity.
One of the most common downstream consequences of this immune activation is the development of food sensitivities. When larger food particles cross a compromised gut barrier and interact with the immune system, they can trigger reactions in susceptible people. That doesn’t mean you’re suddenly allergic to everything, but it does mean your immune system is working overtime. In both my practice and personal experience, I’ve seen many food reactions soften or resolve as we heal the gut, remodulate the immune system, and calm inflammation.
The Good News and Hard News
The good news is that the same strategies that address dysbiosis and leaky gut also tend to lower systemic inflammation, calm immune overactivation, and improve autoimmune symptoms. In other words, these are not separate problems that require separate solutions; they are different faces of the same underlying process.
At the same time, understanding how intertwined these pieces are explains why quick fixes rarely work. You can’t simply add a probiotic and expect resolution if the gut lining remains compromised. You can’t fully heal the gut lining if inflammatory signals are continuously undermining repair. And you can’t resolve chronic inflammation if dysbiosis keeps feeding endotoxins and other immune triggers into the bloodstream.
Ultimately, piecemeal approaches often fail. True progress usually requires addressing all three simultaneously and systematically using the 5R approach:
-
- Removing the triggers that drive dysbiosis and permeability
- Replacing or restoring enzymes, stomach acid, and depleted nutrients needed for proper digestion
- Reinoculating or rebalancing microbial diversity
- Repairing the gut barrier
- Rebalancing your lifestyle to reduce stress and inflammatory load
It also requires patience; while the gut lining can begin to repair in weeks, fully rebalancing a disrupted microbiome typically takes months, not days.
In my next post, I’ll walk you through the first practical steps to begin healing leaky gut: how to lower inflammatory load, choose foods that support your microbiome, and gently interrupt this vicious cycle so your body can start to repair.
Don’t miss the next post—subscribe to Wednesday’s Wisdom and Wellness now to get practical steps, Scripture, and anti-inflammatory recipes delivered to your inbox weekly.
Join the newsletter below.
No spam. Unsubscribe anytime.