Most sleep advice focuses on screens, stress, and bedtime routines. But what you eat—and specifically how much fiber you’re getting—may be quietly shaping how well you sleep each night.
Research increasingly points to a connection between dietary fiber and sleep quality. It’s not a simple one‑to‑one relationship, but the mechanisms are biologically plausible and supported by early human studies. It’s enough to be worth understanding if you’re waking at 2 a.m., struggling to fall asleep, or never quite feeling rested.
Let’s walk through what the science actually says.
How Fiber and Sleep Connect Through the Gut–Brain Axis
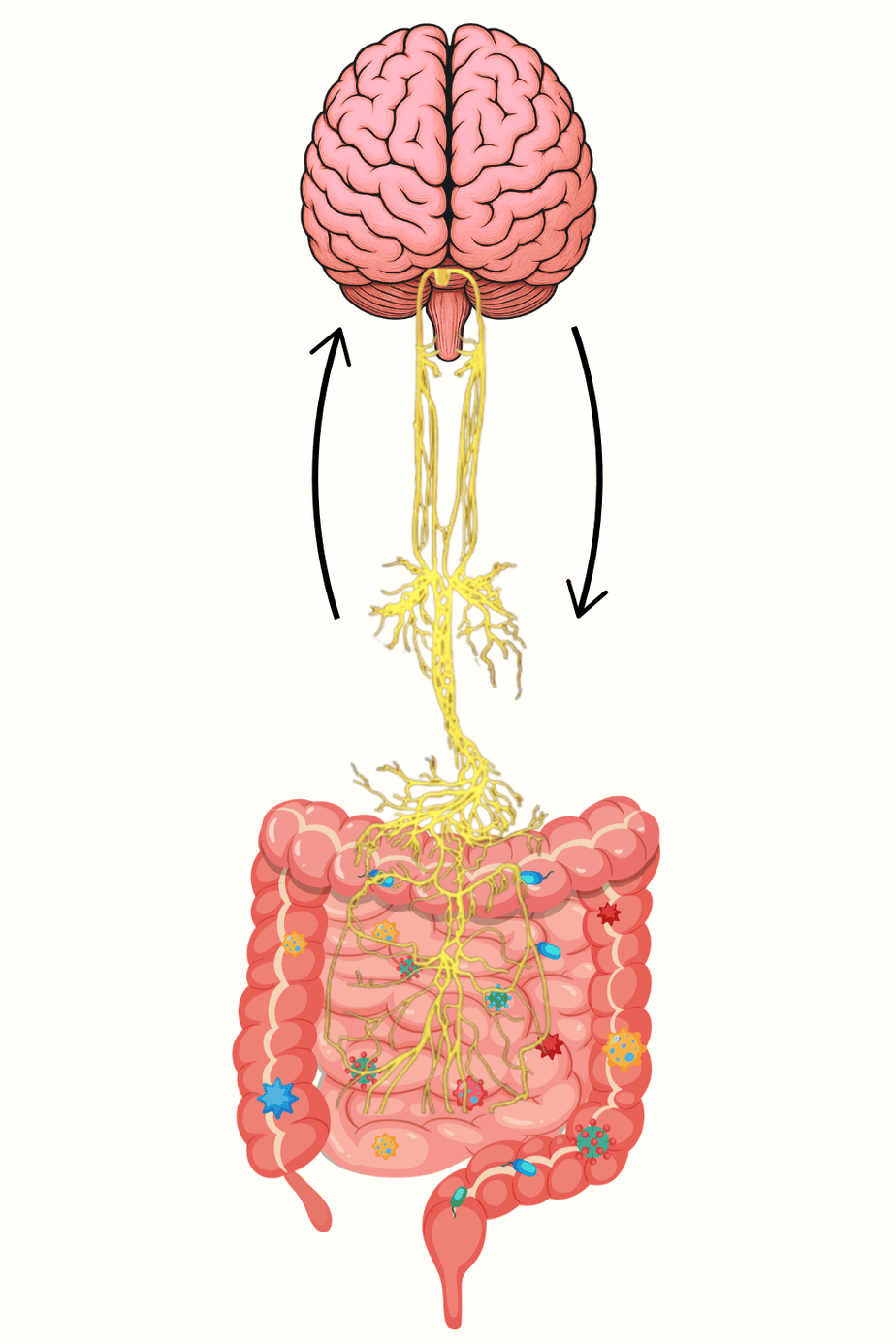
Your gut and brain are in constant communication through a network of nerves, hormones, and chemical signals. That gut–brain communication is a big part of the link between fiber and sleep. One of the less obvious ways it influences sleep is through the microbes living in your digestive tract.
When you eat fiber, particularly fermentable fiber from vegetables, fruits, legumes, and whole grains, your gut bacteria ferment it and produce short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate. These aren’t just byproducts. They’re signaling molecules that communicate with your immune system, your gut lining, and your brain.
Here’s where sleep enters the picture: SCFAs influence the production of neurotransmitters that regulate your sleep-wake cycle. Roughly 90% of your body’s serotonin is produced in the gut, and serotonin is a precursor to melatonin—the hormone that signals your brain it’s time to sleep. A well-nourished microbiome supports this entire chain.
Additionally, fiber helps nourish gut bacteria that may influence GABA, a calming neurotransmitter that quiets nervous system activity at night. When your microbiome is depleted—through low fiber intake, stress, or antibiotic use—these neurotransmitter pathways can become disrupted, making it harder to wind down and stay asleep.
Blood Sugar Stability and Nighttime Awakenings
Have you ever woken up at 2 or 3 a.m. feeling wired, anxious, or unable to get back to sleep? While it’s not the only cause, blood sugar instability is one common—and often overlooked—reason this happens.
When blood sugar drops too low overnight, your body responds by releasing cortisol and adrenaline to bring it back up. These are stress hormones designed to rouse you into action, which is exactly what they do. They pull you out of deep sleep in the middle of the night.
Fiber slows carbohydrate digestion and blunts the post-meal blood sugar spikes and crashes that set this cycle in motion. Soluble fiber in particular, such as what’s found in oats, legumes, chia seeds, flaxseed, and low-glycemic fruits, forms a gel in the digestive tract that slows glucose absorption. Consequently, your blood sugar rises more gradually after meals and stays more stable through the night. This reduces the likelihood of those cortisol-driven wake-ups.
Evening meals that include adequate fiber, healthy fat, and protein are especially important for maintaining overnight blood sugar stability. A high-carbohydrate, low-fiber dinner is essentially a setup for a middle-of-the-night cortisol surge.It doesn’t take a fiber-heavy meal to prevent this. A balanced plate with vegetables, a reasonable serving of whole grains or legumes, and quality protein does the job.
For a deeper dive into how fiber affects GLP-1, insulin sensitivity, and appetite cues, see Fiber and Blood Sugar Regulation: The Natural GLP-1 Connection.
Inflammation, Fiber, and Sleep Quality
Chronic, low-grade inflammation is one of the most consistent findings in people with poor sleep. The relationship runs in both directions: poor sleep drives inflammation, and inflammation disrupts sleep. For many people, it becomes a frustrating cycle.
High-fiber, plant-rich eating patterns are consistently associated with lower levels of inflammatory markers like C-reactive protein and interleukin-6. This happens through several pathways:
-
- Better gut barrier integrity (which reduces the inflammatory signaling triggered by an increased intestinal permeability or “leaky gut”)
- Higher SCFA production
- Lower overall oxidative stress
What does this mean for sleep? Several studies suggest that lower systemic inflammation is associated with more time in slow-wave sleep. This is the deep, restorative stage where physical repair and memory consolidation happen. It’s the stage most people are shortchanged when their sleep is poor.
Ultimately, reducing chronic inflammation through a high-fiber diet isn’t a quick fix, but it’s one of the most sustainable ways to improve your sleep over time.
How Much Fiber Seems Helpful for Sleep?
There’s no magic “sleep dose” of fiber, and the research isn’t at the point of issuing specific sleep-focused recommendations. What we do know is that most American adults fall significantly short of general fiber recommendations. Average fiber intake is just 15 to 16 grams per day. Recommended intake is 14 grams per 1,000 calories of food. Since men generally need more calories and older adults need fewer, the following chart shows recommendations based on gender and age.
Observational studies tell an interesting story. A small inpatient study published in the Journal of Clinical Sleep Medicinefound that higher daytime fiber intake was associated with more time in deep, slow‑wave sleep and fewer arousals that night. Conversely, lower fiber intake was associated with lighter, less restorative sleep and more frequent waking.
The practical takeaway: most people aren’t eating enough fiber for their gut health generally, let alone for optimal sleep. Gradually moving toward (or slightly above) the standard daily targets is a reasonable and well-supported goal. Importantly, gradual is the key word here, especially if your gut is sensitive. Too much fiber added too quickly can cause gas and bloating that disrupts sleep in its own way.
Best Fiber Sources for Sleep-Supportive Meals
Not all fiber works the same way in the gut, and variety matters. A diverse range of fiber sources supports a more diverse microbiome. In turn, that supports a richer blend of SCFAs and neurotransmitter precursors.
For sleep specifically, the most relevant fiber sources are those that ferment slowly and feed the bacteria most involved in SCFA and serotonin production:
Legumes (lentils, black beans, chickpeas, white beans) are among the richest sources of prebiotic fiber and are exceptionally good at feeding butyrate-producing bacteria.
Intact whole grains (oats, brown rice, quinoa, millet, buckwheat) provide both soluble and insoluble fiber and are digested more slowly than refined grains, supporting overnight blood sugar stability.
Vegetables, especially leafy greens, root vegetables, and cruciferous vegetables, contribute a variety of fibers and polyphenols that support microbiome diversity.
Bonus Tip: Cooking and then chilling legumes, potatoes, pasta, and rice converts some of their starch into resistant starch through a process called retrogradation, making them even more beneficial for your gut microbiome. See Lentil Meal Prep: One Batch of Lentils, Three Family Meals for more on how this works.
Fruits, particularly berries, apples, pears, and kiwi, add soluble fiber and antioxidants. Kiwi in particular has been studied for its potential sleep‑supportive effects, likely related to its serotonin, melatonin, and antioxidant content.
Nuts and seeds — chia, flaxseed, pumpkin seeds, and almonds — provide fiber along with magnesium, which plays a direct role in sleep regulation.
Practical Ways to Boost Fiber for Better Sleep
You don’t need to overhaul your entire diet to see a difference. Strategic changes to your evening pattern and a gradual ramp-up overall are often enough to move the needle.
- Build a fiber-forward dinner plate. Use the Anti-Inflammatory Rainbow Diet (AIRD) as a simple template: aim for roughly half your plate from non-starchy vegetables, a quarter from lean protein, and a quarter from whole-food starches like legumes, intact whole grains, or starchy vegetables. This structure naturally delivers meaningful fiber without obsessive tracking.
- Add a smart pre-bedtime snack if needed. If you tend to wake up in the early hours, a small snack before bed that combines fiber with protein and healthy fat can help stabilize blood sugar overnight. Options include a small handful of pistachios, half of an apple with almond butter, or 1/4 to 1/3 cup of plain Greek or goat yogurt with berries and a sprinkle of chia seeds. Keep portions small. The goal is stability, not a full meal.
- Ramp up gradually if your gut is sensitive. Increasing fiber too quickly is a common mistake. Allow your microbiome time to adapt by adding roughly 3 to 5 grams of additional fiber per week and be sure to increase water intake at the same time. This significantly reduces the likelihood of constipation, gas, bloating, and discomfort that derail well-intentioned efforts.
- Front-load your fiber earlier in the day. Eating high-fiber meals right before bed can cause discomfort for many people, and it forces our body to work on digestion instead of rest and repair. So, keep evening meals moderately fibrous, and focus on breakfast and lunch for easily building fiber intake. Think: oatmeal with chia and berries, a big salad with legumes, a gluten-free grain bowl with roasted vegetables or one of these delicious bowl recipes:
Brisket Bowl with Roasted Veggies and Lemon Tahini Sauce
- Try a 5-day fiber experiment. Commit to hitting 25+ grams of fiber per day for five days and pay attention to how you sleep. Keep a simple sleep log that includes time to fall asleep, any wake-ups, how rested you feel in the morning. Changes in sleep patterns can take a week or two to show up, but many people notice something within days, particularly if blood sugar instability has been driving their nighttime awakenings.
The Bigger Picture
Fiber and sleep sit at the intersection of gut health, blood sugar regulation, and inflammation—three areas that functional nutrition has always understood as deeply connected. Improving one tends to improve the others.
So, if you’re consistently waking at 2 or 3 a.m., relying on sleep aids, or waking unrefreshed despite a full night in bed, exploring fiber and sleep could be the simple change you’ve been missing.
Curious whether gut health or blood sugar instability might be at the root of your sleep struggles? Schedule a free 30-minute strategy session and let’s take a look at the full picture.
Want weekly Scripture, wellness tips, and anti-inflammatory recipes?
Subscribe to the newsletter below.
No spam. Unsubscribe anytime.