Hippocrates said, “All disease begins in the gut.” Dr. Alessio Fasano said, “It’s all about the leaky gut.” I believe they were both right, and I’ve learned that lesson through both personal and clinical experience: if you don’t heal the gut, you’re swimming upstream trying to fix anything else. In this post, I’ll walk you through how to heal leaky gut with five practical steps—and how to personalize them for your unique situation.
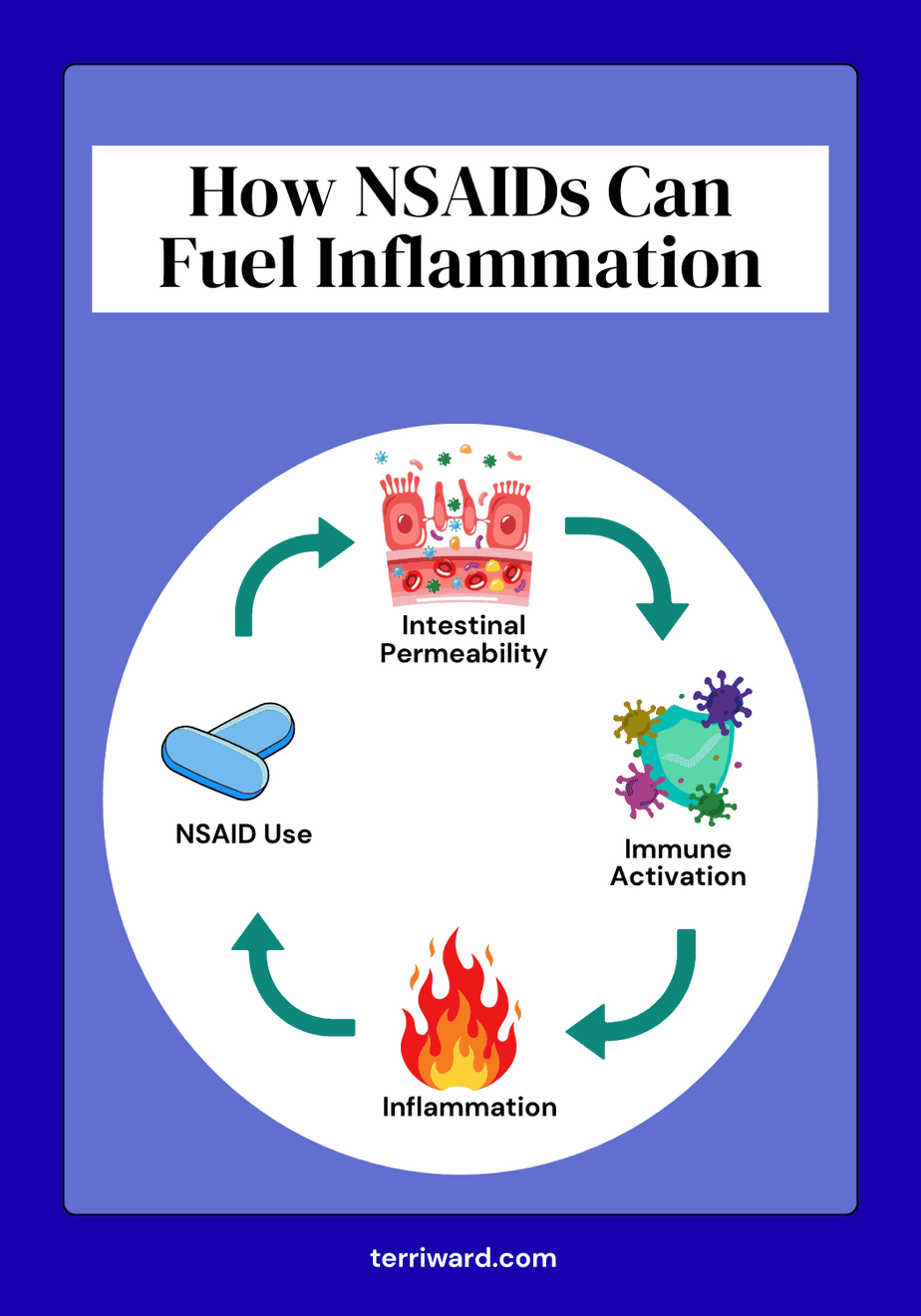
For years, my gut was a mess, and I had no idea gluten was keeping it inflamed and leaky. Leaky gut, or intestinal permeability, is exactly what it sounds like: a compromised gut lining that allows undigested food particles, microbes, and other substances to slip into the bloodstream and activate the immune system.
Before diving into healing, you might want to check out these posts for the full picture of what leaky gut is, what causes it, and why it’s often connected to persistent symptoms:
Intestinal Permeability: What Leaky Gut Is (and Isn’t)
Leaky Gut and Inflammation: The Vicious Cycle with Dysbiosis
Researchers increasingly recognize that intestinal permeability is common. However, its true prevalence is unclear because it’s rarely tested in routine practice. Additionally, many symptoms aren’t recognized as gut related—even by clinicians. In Part Two of my book God’s Prescription, I explain how leaky gut contributes to inflammation and how everything is connected. From mental health and bone health to skin issues and heart health, starting with gut healing can shift many of these problems.
Signs You May Have Leaky Gut
How do you know if you have leaky gut? The symptoms are often hiding in plain sight. Bloating, gas, and unpredictable digestion are common, but so are symptoms that seem unrelated to the gut, such as brain fog, joint pain, skin conditions, fatigue, and mood disturbances. If you have an active autoimmune disease or frequent food reactions, research strongly suggests leaky gut is likely part of the picture. Increased intestinal permeability is widely recognized as a prerequisite for autoimmune disease development.
How to Heal Leaky Gut using Functional Medicine’s 5Rs
The 5Rs of functional medicine are well established, but how they are applied is as individual as your gut microbiome.
Everyone wants to jump straight to probiotics and gut-healing supplements. But if you’re still lighting your immune system on fire, you’re wasting your time and money.
Imagine your gut as a boat with holes in it. It doesn’t make sense to keep bailing water while drilling new holes in the hull.
When we mask symptoms by interfering with a natural bodily process, we’re not fixing the holes—we’re just temporarily managing the flooding. For example, taking a non-steroidal anti-inflammatory drug (NSAID) such as ibuprofen, Aleve, or Celebrex blocks the body’s inflammatory signals, but it doesn’t remove the underlying cause of the inflammation. When the drug wears off, the problem is still there. In fact, repeated use can further damage the gut barrier, creating a vicious cycle.
Before the gut can heal, you must first eliminate the obstacles interfering with the body’s natural ability to function as God intended. The goal isn’t to make leaky gut more tolerable—it’s to remove what’s driving it.
That’s why the first step in the 5R framework is Remove.
Step 1: Remove – Stop Poking Holes in the Boat
In functional medicine, this step focuses on identifying and removing the most common drivers of intestinal permeability and gut inflammation.
Remove (or reduce) gut-damaging medications where possible:
Certain medications are known to increase intestinal permeability, including non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and Aleve as well as acid-suppressing medications and some other drugs. Never stop a prescription medication without speaking to your prescribing practitioner.
When talking to your practitioner, avoid using the phrase leaky gut or you might be dismissed. Instead, ask about intestinal permeability or damage to the gut barrier, which are well documented.
Remove infections and overgrowths:
Parasites, yeast, and overgrowth of opportunistic bacteria can all contribute to gut inflammation and barrier damage. Comprehensive stool testing can help identify these organisms so they can be addressed with targeted herbal or prescription treatments.
Remove inflammatory trigger foods:
Common triggers include gluten, dairy, soy, sugar, fast food, ultra-processed foods, and seed oils. An elimination diet can often help identify problem foods. But when reactions are widespread or confusing, testing can sometimes provide useful clues.
For example, when I experienced uranium toxicity, I developed reactions to many foods that I couldn’t easily identify on my own. A food allergy and sensitivity panel revealed allergic (IgE) reactions to beans and eggs and sensitivity (IgG) reactions to beef, oats, and lamb. I never suspected I had any IgE reactions, nor did I ever suspect beef and lamb were culprits. It wasn’t easy, but I sure felt better when I eliminated all of those foods.
If you’re tempted to skip this step and jump to fancy powders and capsules, don’t. Until you stop what’s poking holes in your gut lining, you’re just bailing water out of a leaking boat.
Step 2: Replace – Give Your Gut What It’s Missing
Modern life is very good at interfering with the natural production of things our bodies need to function properly. That includes key components of digestion such as stomach acid, digestive enzymes, and bile.
Thus, the replace step is about restoring what your body needs to break down food properly so it’s less irritating by the time it gets to that vulnerable intestinal lining that’s only one cell layer thick.
An easy, free tip to help stimulate digestion is to chew your food thoroughly, which mechanically breaks food down while saliva begins the chemical digestive process with enzymes.
For those who need supplemental support, the following can be transformational:
Stomach acid
Low stomach acid is incredibly common, especially with chronic stress and acid blockers. Carefully restoring stomach acid can improve protein digestion and reduce irritation further down the digestive tract.
Digestive enzymes
Targeted supplemental enzymes can help break down proteins, fats, and carbohydrates more completely so fewer large food particles slip through a leaky gut and trigger an immune reaction.
Bile salts
If you’ve had your gallbladder removed or struggle with fat digestion, your gut may need extra help emulsifying fats so they can be properly absorbed.
Nutrients involved in digestion:
B vitamins, zinc, and magnesium may be deficient or insufficient in some individuals and can play an important role in digestive function.
A comprehensive stool analysis really shines here. It provides markers such as pancreatic elastase, fecal fats, and short-chain fatty acids so we don’t have to guess whether you’re digesting fats or proteins well. That data helps identify what might be missing so we’re not just guessing.
Step 3: Reinoculate – Choose Probiotics Wisely
This is the step in the 5R framework that often gets reduced to “take a probiotic.” But reinoculation is more intentional than that.
It involves two things:
1. Reintroducing beneficial microbes through probiotics and, in some cases, fermented foods:
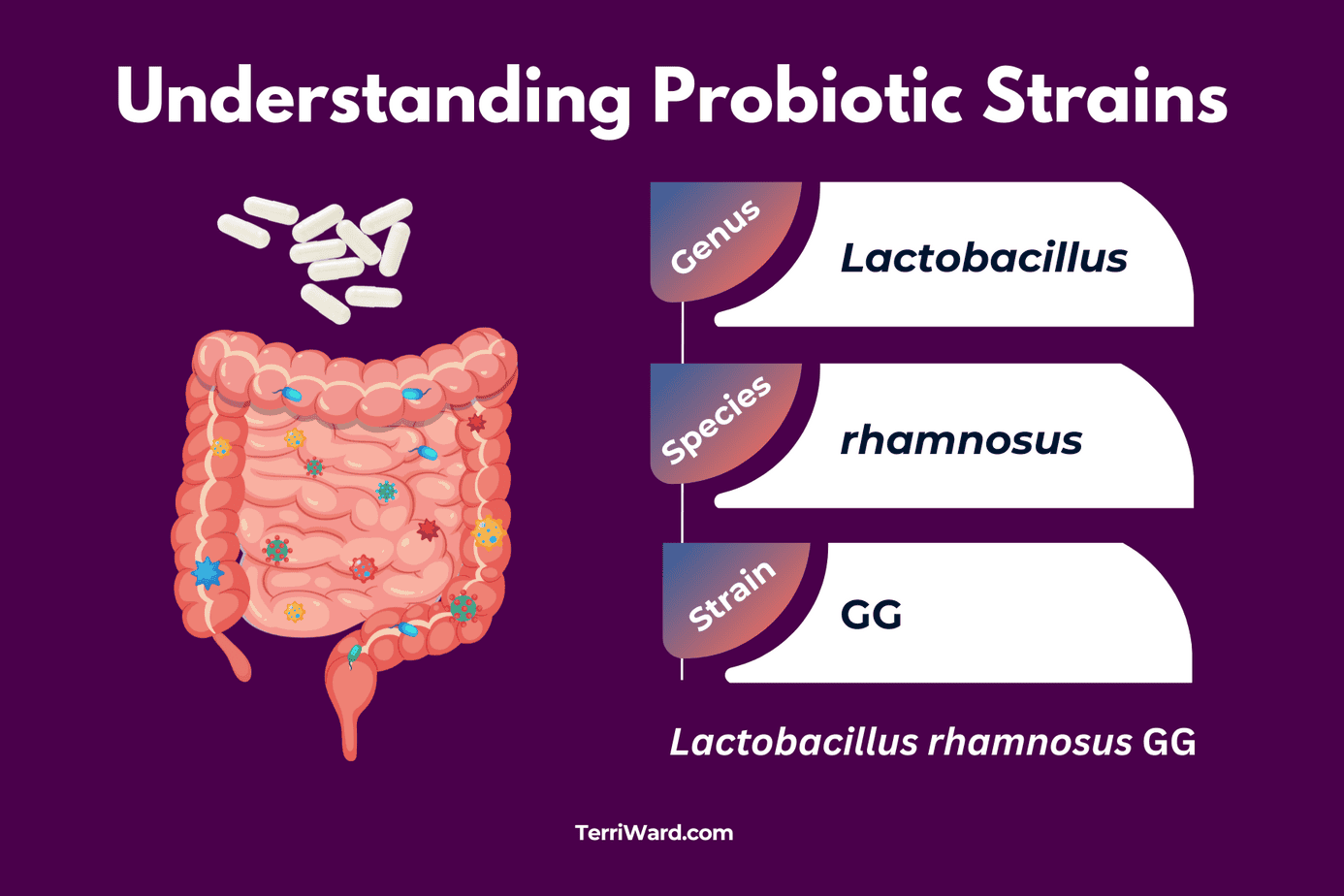
However, not all probiotics are created equal, and not all strains have the same effects. Many supplement labels only disclose the genus and species while keeping the specific strain proprietary. But research showing benefits almost always applies to a specific strain, not the entire species.
Because of that, it’s best to work with a knowledgeable practitioner who understands what specific strains do and employs testing rather than guessing. A comprehensive stool analysis can reveal the actual composition and balance of gut bacteria. Otherwise, people often grab a random multi-strain product and hope one of those bacteria helps while the others irritate an already inflamed gut.
Regularly consuming fermented foods such as raw sauerkraut, kimchi, and kefir can be a safer way to introduce beneficial microbes than randomly experimenting with probiotic supplements.
Another important point is that probiotics usually don’t permanently colonize the gut. Instead, they influence the microbial environment as they pass through the digestive tract. Because of that, it can be just as important—sometimes more important—to feed the beneficial bacteria already living in your gut.
2. Feeding beneficial microbes with fiber and other prebiotic foods:
Prebiotic foods contain fibers that beneficial gut bacteria use as fuel. Examples include foods like onions, garlic, leeks, asparagus, apples, oats, legumes, and resistant starch from cooked and cooled potatoes or rice.
Step 4: Repair – Actually Heal the Gut Lining
Did you know your gut lining renews itself every few days? That’s not an accident—that’s design. You were built with a capacity to heal. Once you stop poking holes in the boat, healing can begin while digestion improves and your microbiome rebalances. But healing damaged tissue still requires the right building blocks and anti-inflammatory support.
Supportive nutrients may include:
-
- Zinc carnosine, vitamins A and D, collagen peptides, quercetin, omega-3 fatty acids, and butyrate support mucosal integrity and healthy immune regulation.
- Amino acids like L-glutamine fuel intestinal cells and support repair of the gut lining.
- Soothing botanicals such as marshmallow root, slippery elm, deglycyrrhizinated licorice (DGL), and aloe (in non-laxative preparations) may help calm irritated mucosal tissue. Individuals with autoimmune conditions should consult their healthcare professional before using DGL.
Step 5: Rebalance – Live Like You Want Your Gut to Last
This is the step many protocols reduce to “maintain a balanced lifestyle.” But real healing requires more than a temporary protocol. It requires habits that support your body for the long term.
Science-backed practices that help rebalance the gut and support lasting health include:
-
- Prayer, gratitude, meditation, and mindfulness practices. Even pausing to give thanks for a meal can shift the nervous system into a state more conducive to digestion.
- An anti-inflammatory, nutrient-dense diet. Whole foods rich in vitamins, minerals, fiber, and healthy fats help maintain microbial balance and support the integrity of the gut barrier.
- Managing stress and creating margin. Chronic stress increases intestinal permeability and disrupts digestion. You cannot hate your body, run it into the ground, and expect a calm, resilient gut. A pace of life with no margin for rest is a hormonal nightmare.
- Sleep is not a luxury. It’s when your body repairs tissues, regulates immune function, and recalibrates hormones that influence gut motility and barrier integrity. Honoring your circadian rhythms is an act of stewardship.
- Movement. Regular, moderate movement supports healthy gut motility, circulation, and insulin sensitivity—all of which influence the gut. But more isn’t always better. Excessive or intense exercise can actually increase intestinal permeability.
Where to Go from Here
How much longer are you willing to keep trying supplements or chasing the latest online protocol? Identifying your individual triggers and implementing a personalized plan can create transformation in weeks or months rather than years. The 5R framework is well established, but it works best when it’s applied strategically based on your history, diet, lifestyle, and—when appropriate—objective testing.
If you’d like help identifying what may be interfering with gut healing in your case, schedule a free 15‑minute chat here, and we’ll explore your next best steps.
Because you weren’t designed to live with a chronically leaky, inflamed gut that keeps creating new problems.
Want weekly Scripture, wellness tips, and anti-inflammatory recipes?
Subscribe to the Wednesday’s Wisdome and Wellness newsletter below.
No spam. Unsubscribe anytime.